 Windsor Clinic: 0800 644 0700 -
Reading Clinic: 0800 644 0900
tannereyes@sapphire-eyecare.co.uk
Windsor Clinic: 0800 644 0700 -
Reading Clinic: 0800 644 0900
tannereyes@sapphire-eyecare.co.uk
 Windsor Clinic: 0800 644 0700 -
Reading Clinic: 0800 644 0900
tannereyes@sapphire-eyecare.co.uk
Windsor Clinic: 0800 644 0700 -
Reading Clinic: 0800 644 0900
tannereyes@sapphire-eyecare.co.uk

Mr Tanner has recently introduced new techniques allowing incision size to be decreased to less than 2mm. These small incisions seal themselves immediately after surgery without stitches and normal daily activities can be resumed soon after surgery. Another advantage of no-stitch incisions is that they do not cause a focusing problem known as astigmatism.
After the incision has been made a round opening is created in the lens capsule. A phacoemulsification probe is then inserted, breaking the lens into tiny pieces which are sucked out of the eye. Phacoemulsification uses high-speed ultrasound waves, vibrating 40,000 times per second. Ultrasound phacoemulsification is quicker and safer than a laser to remove the natural lens.
A lens implant is then placed in the lens capsule to replace the focus power of the natural lens. The latest preoperative measuring and surgical techniques allow 90-95% of people to be independent of distance spectacles following refractive lens exchange. It is also possible to insert multifocal lenses helping to correct for the need for reading spectacles.
Mr Tanner will be able to advise you on the latest developments in intraocular lens technology and which models are most appropriate on an individual basis.
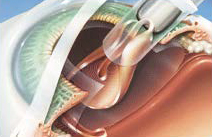
A replacement intraocular lens is inserted and then unfolded in the eye
Lens surgery is a painless experience and the vast majority of operations are now done as a day case procedure. Mr Tanner uses two kinds of anaesthesia – topical anaesthesia and regional anaesthesia.
Topical anaesthesia is very popular with many people because no needles are required. Instead, painless drops are used to numb the eye. No eye patch is needed and patients usually notice improved vision after 24 hrs.
Sub-tenons anaesthesia involves gently injecting a local anaesthetic into the tissues around the eye. The eye is patched for the rest of the day and patients usually notice improved vision after 24-48 hours.
Topical anaesthesia is Mr Tanner’s preferred technique as it offers a quicker recovery with fewer side effects and is completely pain free. The eye is fully anaesthetised but otherwise, you are awake during the procedure, which takes about 15 minutes.
The operation is usually performed as a ‘day case’, shortening the time in hospital and reducing expense for the patient. Local anaesthesia also avoids the post-operative ‘hangover’ from a general anaesthetic, as well as avoiding the risks of an anaesthetic in patients with, for example, chest problems. Of course, general anaesthesia is still available for patients who prefer to be completely asleep. Many patients worry that they will see what is happening during the operation but all that people usually notice is a bright light and vague shapes. Although you have to lie fairly still, there is no need to be rigidly immobile; you can adjust your position or even cough or sneeze, provided some warning is given.
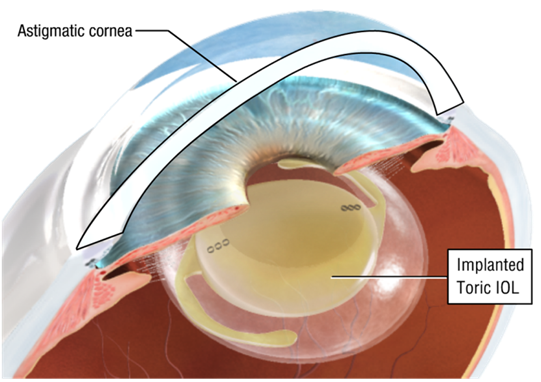
Refractive lens surgery
Many advances in recent years have made the operation safer and improved visual outcome. However, you should be aware that there is a small risk of complications, either during or after the operation. Complications are usually treatable, possibly requiring further surgery. In a few cases serious problems such as infection or retinal detachment occur which may result in visual loss. Mr Tanner runs a continuous audit programme and his results are consistently better than national benchmark data.
One of the commonest problems following lens surgery is the development of posterior capsule opacification as a reaction to the presence of the lens implant. This can result in blurring of vision but is easily treated as an out patient laser procedure.
Greater Clarity of Vision: Vision is crisper and sharper.
Improved Quality of Life: Many studies have shown that people enjoy improved quality of life after successful lens replacement surgery. Most people feel that driving and activities such as reading, sewing, golf and using a computer are all much easier without the requirement for contact lenses or glasses.
Toric Lenses – Removal of astigmatism: Newly developed Toric lenses allow the power of the lens to be different at different orientations within the eye. This allows correction of abnormal corneal curvature, known as astigmatism, and increases independence from spectacles post-operatively.
Multifocal lenses – No reading glasses: These lenses offer the potential to see well for near and distance without the use of glasses following lens surgery in selected cases. Many people are delighted with this option but it does have some drawbacks, including possible haloes around lights at night. Mr Tanner will discuss the relative merits and whether or not a multifocal lens is appropriate for you on an individual basis.
Remaining Glasses Requirement: Eye measurement and lens technology are continuingly improving and the vast majority of patients find that they no longer require glasses or contact lenses for the majority of activities. It is impossible to guarantee that no glasses or contact lenses will be required but around 90-95% of patients achieve spectacle independence following surgery. If one of the gentle multifocal lenses are used, then this usually enables around 90% of activities to be carried out without reading spectacles with occasional use of glasses for smaller print in dim light.
Mr Tanner and his team are very happy to discuss any questions you may have regarding potential refractive lens exchange surgery.
For more information, please visit www.tanner-eyes.co.uk which has many patient information leaflets and background information on the latest lenses available.
Disclaimer : The information provided in this website is intended as a useful aid to general practitioners, optometrists and patients. It is impossible to diagnose and treat patients adequately without a thorough eye examination by a qualified ophthalmologist, optometrist or your general practitioner. Hopefully the information will be of use prior to and following a consultation which it supplements and does not replace.


